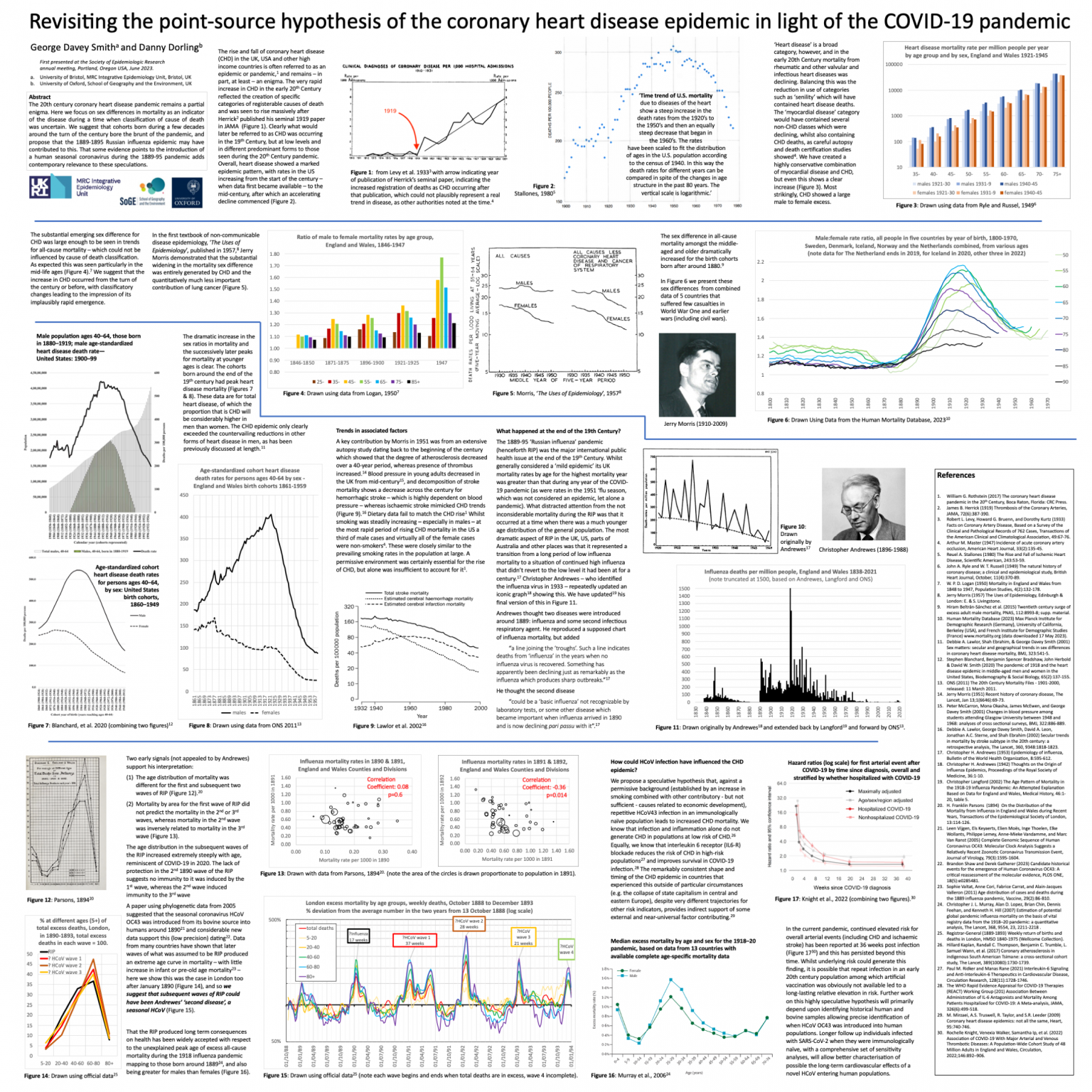
The 20th century coronary heart disease pandemic remains a partial enigma. Here we focus on sex differences in mortality as an indicator of the disease during a time when classification of cause of death was uncertain. We suggest that cohorts born during a few decades around the turn of the century bore the brunt of the pandemic, and propose that the 1889-1895 Russian influenza epidemic may have contributed to this. That some evidence points to the introduction of a human seasonal coronavirus during the 1889-95 pandemic adds contemporary relevance to these speculations. …
George Davey Smith, Society of Epidemiologic Research annual meeting, Portland (Oregon) USA, 14 June 2023, obscuring the key graph (see link below and here for the full sized poster)
…In the current pandemic, continued elevated risk for overall arterial events (including CHD and ischaemic stroke) has been reported at 36 weeks post infection (Figure 17, Reference 30) and this has persisted beyond this time. Whilst underlying risk could generate this finding, it is possible that repeat infection in an early 20th century population among which artificial vaccination was obviously not available led to a long-lasting relative elevation in risk. Further work on this highly speculative hypothesis will primarily depend upon identifying historical human and bovine samples allowing precise identification of when HCoV OC43 was introduced into human populations. Longer follow up individuals infected with SARS-CoV-2 when they were immunologically naïve, with a comprehensive set of sensitivity analyses, will allow better characterisation of possible the long-term cardiovascular effects of a novel HCoV entering human populations.
Click on the image below and open it in a new tab to zoom in.
Or click here for a PDF
 Download PDF (2.7 MB)
Download PDF (2.7 MB)
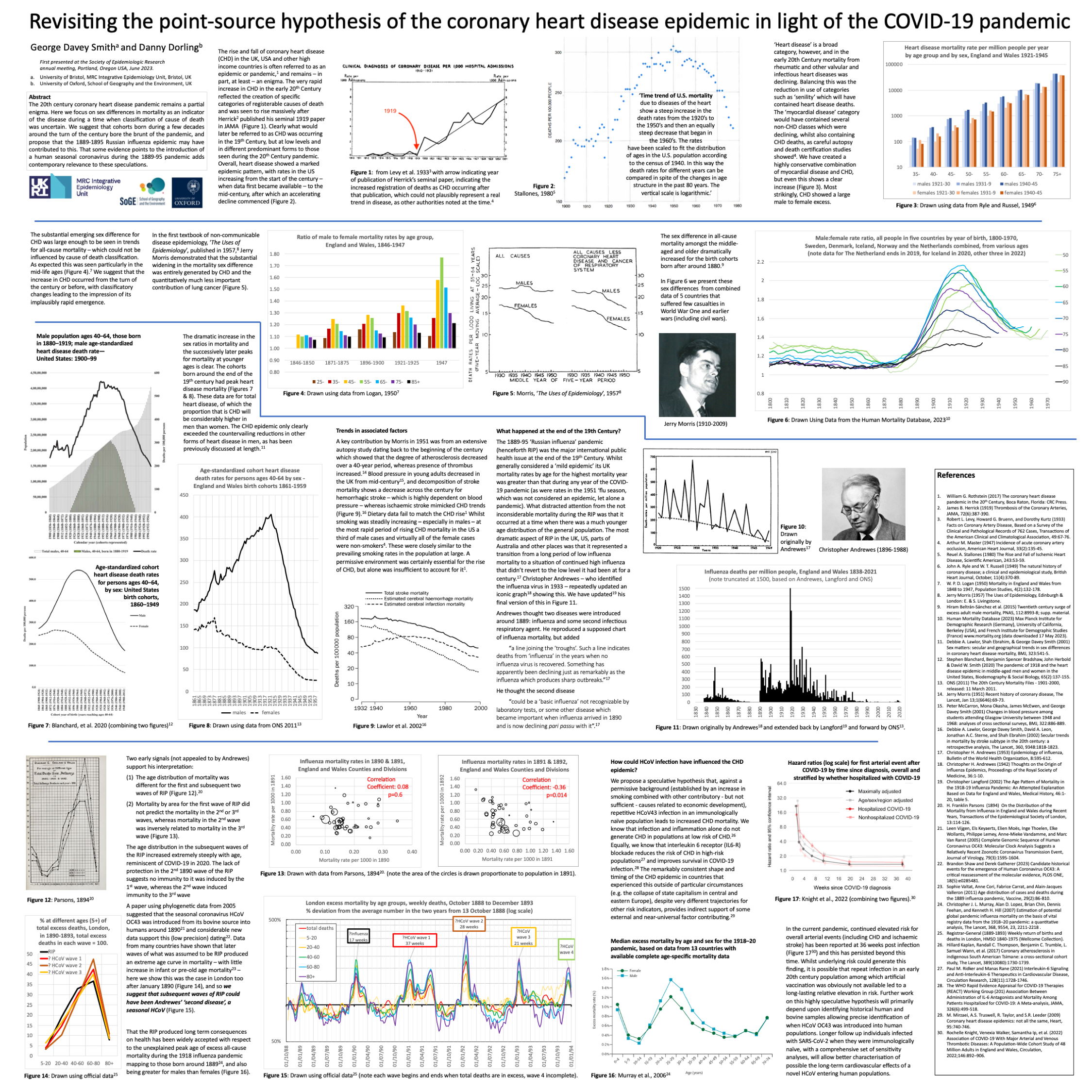
Revisiting the point-source hypothesis of the coronary heart disease epidemic in light of the COVID-19 pandemic
To see the detail in a pdf of the poster, and where it was originally presented click here
References (with embedded links)
1. William G. Rothstein (2017) The coronary heart disease pandemic in the 20th Century, Boca Raton, Florida: CRC Press.
2. James B. Herrick (1919) Thrombosis of the Coronary Arteries, JAMA, 72(6):387-390.
3. Robert L. Levy, Howard G. Bruenn, and Dorothy Kurtz (1933) Facts on Coronary Artery Disease, Based on a Survey of the Clinical and Pathological Records of 762 Cases, Transactions of the American Clinical and Climatological Association, 49:67-76.
4. Arthur M. Master (1947) Incidence of acute coronary artery occlusion, American Heart Journal, 33(2):135-45.
5. Reuel A. Stallones (1980) The Rise and Fall of Ischemic Heart Disease, Scientific American, 243:53-59.
6. John A. Ryle and W. T. Russell (1949) The natural history of coronary disease; a clinical and epidemiological study, British Heart Journal, October, 11(4):370-89.
7. W. P. D. Logan (1950) Mortality in England and Wales from 1848 to 1947, Population Studies, 4(2):132-178.
8. Jerry Morris (1957) The Uses of Epidemiology, Edinburgh & London: E. & S. Livingstone.
9. Hiram Beltrán-Sánchez et al. (2015) Twentieth century surge of excess adult male mortality, PNAS, 112:8993-8; supp. material.
10. Human Mortality Database (2023) Max Planck Institute for Demographic Research (Germany), University of California, Berkeley (USA), and French Institute for Demographic Studies (France) www.mortality.org (data downloaded 17 May 2023).
11. Debbie A. Lawlor, Shah Ebrahim, & George Davey Smith (2001) Sex matters: secular and geographical trends in sex differences in coronary heart disease mortality, BMJ, 323:541-5.
12. Stephen Blanchard, Benjamin Spencer Bradshaw, John Herbold & David W. Smith (2020) The pandemic of 1918 and the heart disease epidemic in middle-aged men and women in the United States, Biodemography & Social Biology, 65(2):137-155.
13. ONS (2011) The 20th Century Mortality Files – 1901-2000, released: 11 March 2011.
14. Jerry Morris (1951) Recent history of coronary disease, The Lancet, Jan 13;1(6646):69-73.
15. Peter McCarron, Mona Okasha, James McEwen, and George Davey Smith (2001) Changes in blood pressure among students attending Glasgow University between 1948 and 1968: analyses of cross sectional surveys, BMJ, 322:886-889.
16. Debbie A. Lawlor, George Davey Smith, David A. Leon, Jonathan A.C. Sterne, and Shah Ebrahim (2002) Secular trends in mortality by stroke subtype in the 20th century: a retrospective analysis, The Lancet, 360, 9348:1818-1823.
17. Christopher H. Andrewes (1953) Epidemiology of influenza, Bulletin of the World Health Organization, 8:595-612.
18. Christopher H. Andrewes (1942) Thoughts on the Origin of Influenza Epidemics, Proceedings of the Royal Society of Medicine, 36:1-10.
19. Christopher Langford (2002) The Age Pattern of Mortality in the 1918-19 Influenza Pandemic: An Attempted Explanation Based on Data for England and Wales, Medical History, 46:1-20, table 5.
20. H. Franklin Parsons (1894) On the Distribution of the Mortality from Influenza in England and Wales during Recent Years, Transactions of the Epidemiological Society of London, 13:114-126.
21. Leen Vijgen, Els Keyaerts, Elien Moës, Inge Thoelen, Elke Wollants, Philippe Lemey, Anne-Mieke Vandamme, and Marc Van Ranst (2005) Complete Genomic Sequence of Human Coronavirus OC43: Molecular Clock Analysis Suggests a Relatively Recent Zoonotic Coronavirus Transmission Event, Journal of Virology, 79(3):1595-1604.
22. Brandon Shaw and Derek Gatherer (2023) Candidate historical events for the emergence of Human Coronavirus OC43: A critical reassessment of the molecular evidence, PLOS ONE, 18(5):e0285481.
23. Sophie Valtat, Anne Cori, Fabrice Carrat, and Alain-Jacques Valleron (2011) Age distribution of cases and deaths during the 1889 influenza pandemic, Vaccine, 29(2):B6-B10.
24. Christopher J. L. Murray, Alan D. Lopez, Brian Chin, Dennis Feehan, and Kenneth H. Hill (2007) Estimation of potential global pandemic influenza mortality on the basis of vital registry data from the 1918–20 pandemic: a quantitative analysis, The Lancet, 368, 9554, 23, 2211-2218.
25. Registrar-General (1889-1893) Weekly return of births and deaths in London, HMSO 1840-1975 (Wellcome Collection).
26. Hillard Kaplan, Randall C. Thompson, Benjamin C. Trumble, L. Samuel Wann, et al. (2017) Coronary atherosclerosis in indigenous South American Tsimane: a cross-sectional cohort study, The Lancet, 389(10080):1730-1739.
27. Paul M. Ridker and Manas Rane (2021) Interleukin-6 Signaling and Anti-Interleukin-6 Therapeutics in Cardiovascular Disease, Circulation Research, 128(11):1728-1746.
28. The WHO Rapid Evidence Appraisal for COVID-19 Therapies (REACT) Working Group (2021) Association Between Administration of IL-6 Antagonists and Mortality Among Patients Hospitalized for COVID-19: A Meta-analysis, JAMA, 326(6):499-518.
29. M. Mirzaei, A.S. Truswell, R. Taylor, and S.R. Leeder (2009) Coronary heart disease epidemics: not all the same, Heart, 95:740-746.
30. Rochelle Knight, Venexia Walker, Samantha Ip, et al. (2022) Association of COVID-19 With Major Arterial and Venous Thrombotic Diseases: A Population-Wide Cohort Study of 48 Million Adults in England and Wales, Circulation, 2022;146:892–906.


![]() Download PDF (2.7 MB)
Download PDF (2.7 MB)