So what do we know now about Covid-19 in the UK?
It need not have arrived first in Europe in Italy. The disease could have arrived elsewhere on this continent first, and it could have arrived much earlier than it did. Over the course of the past few weeks I have wondered how different the story would have been if a businessman (or woman) from Wuhan, infected but largely asymptomatic, had arrived on New Year’s Eve in Edinburgh and gone for a drink in a packed pub that night. Chance events alter the fate of whole countries, not simply the fate of individuals.
For a ten minute talk discussing the graphs shown here click play below and then scroll down as the talk plays
We know so much more today than we knew when I last wrote in this magazine at the start of the pandemic two months ago. Most importantly we now better know what the risks of mortality are and that, above all else, those risks are related to age. Of all those whose 42,173 people in England and Wales whose death had been registered by May 23rd 2020 as having occurred with Covid-19, some 96% were aged 60 or older. Only 4 people under the age of 15 had Covid-19 mentioned on their death certificate. Some 263 people aged 15-39 had died with Covid-19 or, 0.6% of all those who died (99.4% were 40 or over). Men were more likely than women to die, or putting is another way, men are about as likely to die as a women aged 5 years older than them.
Two graphs are needed to show how the mortality rate varies by age and sex. The first uses a normal scale, which shows clearly that 3% of all men aged 90 or over, and 2% of all women of the same ages, had died with the disease by late May 2020. The second uses a log scale to illustrate just how predictable the rate of mortality is by age.
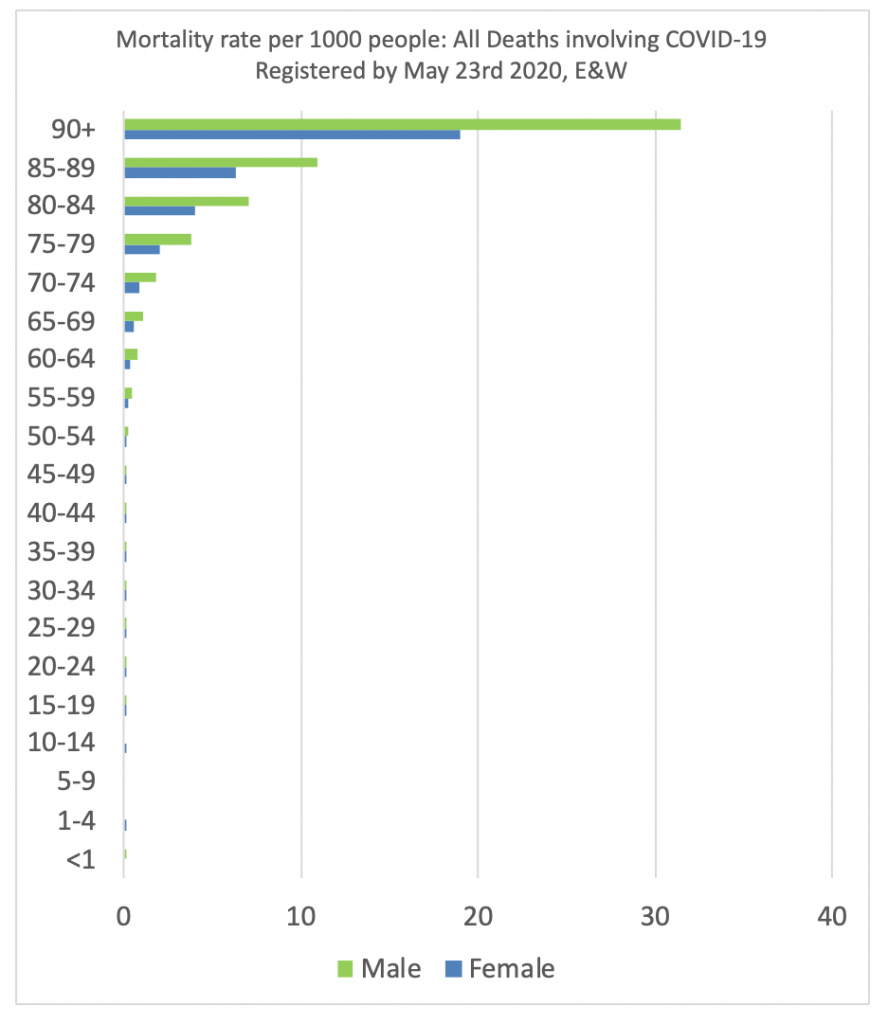
Mortality rate per 1000 people: All deaths involving COVID-19 registered by May 23rd 2020, England and Wales

Mortality rate per 1000 people: All deaths involving COVID-19 registered by May 23rd 2020, E&W – log scale
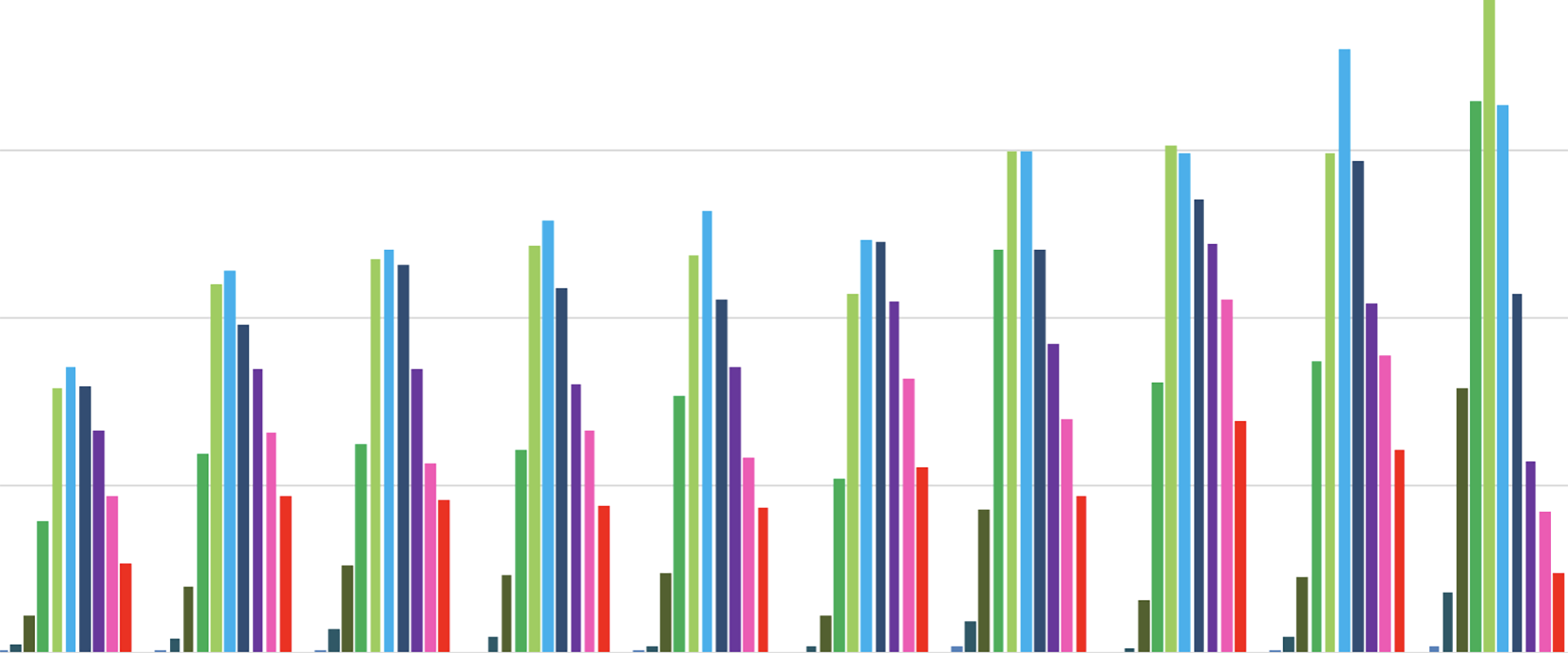
A huge number of reports have been published to give us some idea of what matters other than age: living in an overcrowded household, having to work in a job with close contact to others, living in a part of the country to which the disease came first, being Black or Asian (especially as older Black and Asian people so much more often live in cities to which it came first), and having an underlying poor health condition. However, most important above all is age, and secondly after that – living in England or Wales. The number of people who have died in Scotland or Northern Ireland is much lower. After that, the further you lived away from an urban centre the lower were the mortality rates around you as the next figure shows. It also illustrates that regional mortality rates peaked in London in the week ending April 10th; peaking the next week in the North West of England, but still being almost as high in the week ending April 24th across the less urban South East and South West of England.

Deaths with COVID-19 by region and week of occurrence, E&W rates per million people, by week ending on the date given in the key
The amalgamation of these ten regional curves (even sharper ones that can be seen in particular cities) means that the national epidemic curve for Covid-19 has an elongated shape. The numbers of people dying falling more slowly than they rose, as the next national graph shows. The graph also suggests that social distancing before the lockdown, and partly the lockdown itself, will have affected the shape of this curve. However, there have been no times when there has been a sudden fall in mortality number that could be attributed to a particular change in policy occurring two or weeks earlier. In hindsight, given that the first recorded deaths where Covid-19 is mentioned occurred in very early March all around the country, the disease was clearly widespread in February in both England and Wales.

Deaths with COVID-19 by date of occurrence of death, all registrations up to May 23rd 2020, E&W
The point of maximum acceleration in mortality nationally was March 31st, the day when Dominic Cummings (an advisor to the Prime Minister who has now achieved something of a public profile) arrived in Durham having fled London with his family. The graph below illustrates why, up until March 31st 2020, had you been privy to the mortality data that has subsequently been released, you might well have concluded that mortality rates were then rising exponentially, especially in central London.

Change in the daily number of deaths with COVID-19 by at of occurrence, all registrations up to May 23rd 2020, E&W
Not everyone who died with Covid-19 mentioned on their death certificate will have died primarily due to Covid-19. At the same time some people will have died of the disease without it have been mentioned on their death certificates, especially early on. The next graph below shows how ‘excess deaths ‘ are estimated by comparing deaths in one year with an earlier year. It shows we had not returned to normal in May but might do by June.

Comparison of two full 70 week cycles – England and Wales weekly mortality records – total deaths each week (all causes)
The disease first peaked in week 13 or 14 of 2020 in the following 13 districts: Broxbourne, Ceredigion, Chiltern, Erewash, Fareham, Lambeth, Newport, Rochford, South Bucks, South Holland, South Staffordshire, Tunbridge Wells, and Wolverhampton. That peaking is shown below in a graph which also highlights the effects of discharging patients from hospitals back to care homes.

Deaths with COVID-19 in areas that peaked first by week, England and Wales
The disease peaked a week later in places such as Liverpool and Brent; but did not peak in Cornwall until week 16 of the year; whereas in County Durham the numbers dying peaked in week 15 but also in week 17; before falling more slowly than elsewhere. Quite why calamity was spread unevenly, and why the numbers dying rose and fell faster in some places will take time to assess. But every bar in these graphs represents a pillar of tragedies and for everyone who has died many others will have survived but been greatly harmed.

Deaths with COVID-19 in Liverpool by week

Deaths with COVID-19 in Brent by week

Deaths with COVID-19 in Durham by week

Deaths with COVID-19 in Cornwall by week
All the data used here was released by ONS and was the most recently available at the time of writing towards the end of May 2020. The final graph, below shows the rise and fall of deaths of people who were living in Westminster Borough, in the heart of London and where so many politicians caught the disease.

Deaths with COVID-19 in Westminster Borough by week
In hindsight, it has now become clear that mortality rates fell at the start of April when the number of infections fell at the start of March, because people (long before central government began to express any sense of urgency) began to change their own behaviour. Twenty five days after the full lockdown was imposed, mortality from the disease in the middle of London had almost halved. The same pattern can be seen in Brent above. This disease was brought under control despite the actions of central government, not because of them; although it may turn out to have been national policy (or lack of it) which lead to so many patients being discharged into care homes with the disease.
For a PDF of this article and a link to the original source click here.