The NHS has been run on the goodwill of its staff for too long
“But once this is done, there must be complete transparency about how the NHS came to be left in this exposed position, how social care had been stripped away, and how those in power will be held accountable.”
Lucinda Hiam, Martin McKee and Danny Dorling
On 31st January 2020, the chief medical officer (CMO) for England confirmed the first two cases of novel coronavirus (covid-19) in the UK. The prime minister, Boris Johnson, addressed the nation at a press conference on 3rd March 2020. Johnson said the UK was “extremely well prepared”: “And let’s not forget, we already have a fantastic NHS… we will make sure the NHS gets all the support it needs.”
Healthcare professionals did not share his confidence that the NHS was prepared. One survey asked doctors, “Do you feel the NHS is well prepared for Coronavirus?”—less than 1% said they did. Meanwhile, news bulletins are reporting health workers’ concerns that the supply of personal protective equipment, or PPE, is inadequate, obsolete, improvised, and in some cases, dangerous, leaving staff, some now threatening to quit, feeling “betrayed.” Much remains unknown about how the pandemic will affect the UK, but what is clear is that a decade of under-funding has left the NHS extremely vulnerable. Worse, repeated warnings about this vulnerability have been ignored.
It is not surprising that those on the frontline feel the NHS is unprepared. Before the first case of covid-19 in the UK on 31st January, data for the preceding four weeks revealed that the highest number of patients had waited in A&E for more than four hours “since records began.” 2,846 people waited more than 12 hours to be seen. These figures represented increases of 20.4% and 353.9% respectively above the same period last year.
Yet, January 2020 was not an exception. Rather, it was the continuation of a trend of worsening health outcomes over the past decade. Our review of health trends in the UK between 2010 and 2020, before covid-19, led us to conclude that things are falling apart. The state has been failing in its most basic duty, to protect the health of its people. Life expectancy has stalled, and for some fallen. So-called “deaths of despair,” from drug overdoses, alcohol related conditions, and suicides are rising in 45-54 year olds. Health inequalities are widening, access to healthcare is worsening, and the number of people who are homeless has risen. The UK was simply not prepared for an epidemic.
Successive governments since 2010 have made their priorities clear, no more so than in the months since the pandemic began. Although Downing Street has contested it, The Times newspaper reported sources claiming that the chief advisor to the prime minister, Dominic Cummings had said “…if that means some pensioners die, too bad”. He is not alone in his reluctance to accept the action the pandemic requires. Similar hesitance to act has been seen in the Trump administration, as one columnist put it: “On Wednesday night the global pandemic met US nationalism.”
The same people that have been in power in the UK for the last decade are now discussing the under-funding and resulting crisis in the NHS as if they had nothing to do with it. Jeremy Hunt, the Health and Social Care Secretary from September 2012 to July 2018, said in a BBC Newsnight interview: ‘”In retrospect, the cuts to social care were…the most silent but also the most devastating.” The devastation was not silent, people did complain loudly—but the British government had not been listening.
NHS workers have, as ever, risen to the challenge, moving away from their families, returning from retirement, working outside of their normal roles, and more than 500,000 others have signed up to be NHS volunteers. The NHS has been run on the goodwill of its staff for too long. For now, we must join together to support the crucial work of all those fighting to control the pandemic. But once this is done, there must be complete transparency about how the NHS came to be left in this exposed position, how social care had been stripped away, and how those in power will be held accountable.
Lucinda Hiam, GP and Honorary Research Fellow, London School of Hygiene and Tropical Medicine. Twitter: @lu_hiam
Martin McKee is professor of European public health at the London School of Hygiene and Tropical Medicine. Twitter @martinmckee
Competing interests: None declared
Read PDF of this opinion or see link to the version on the BMJ website here.
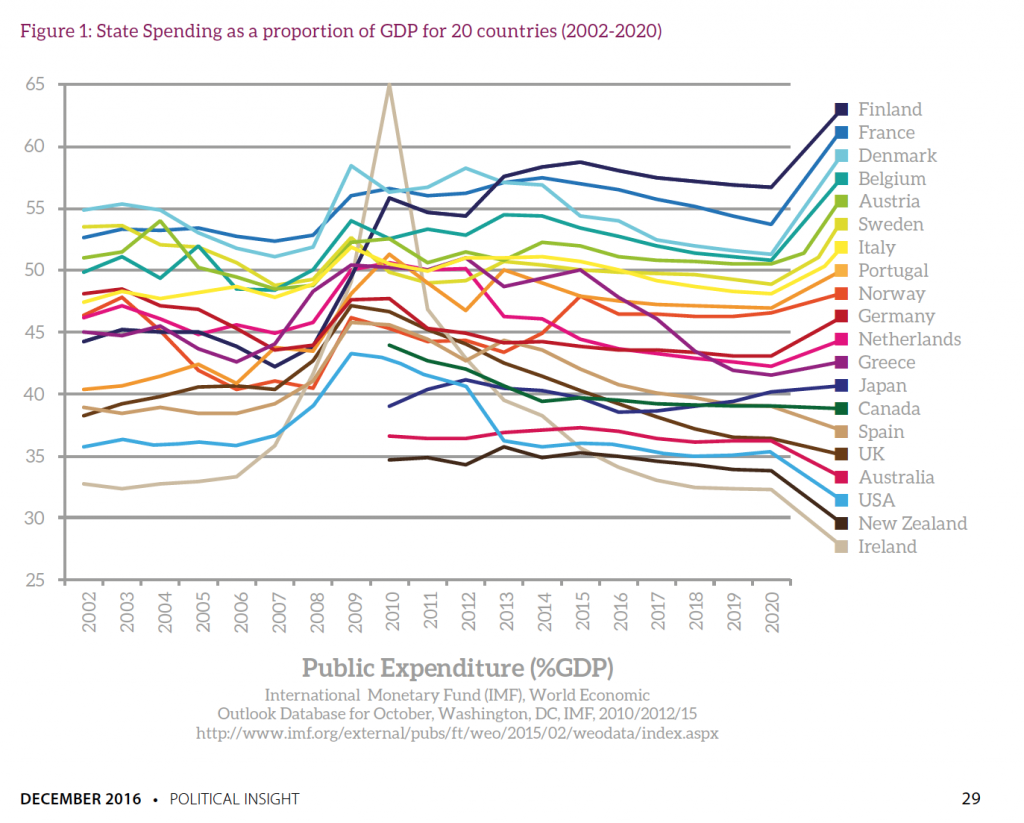
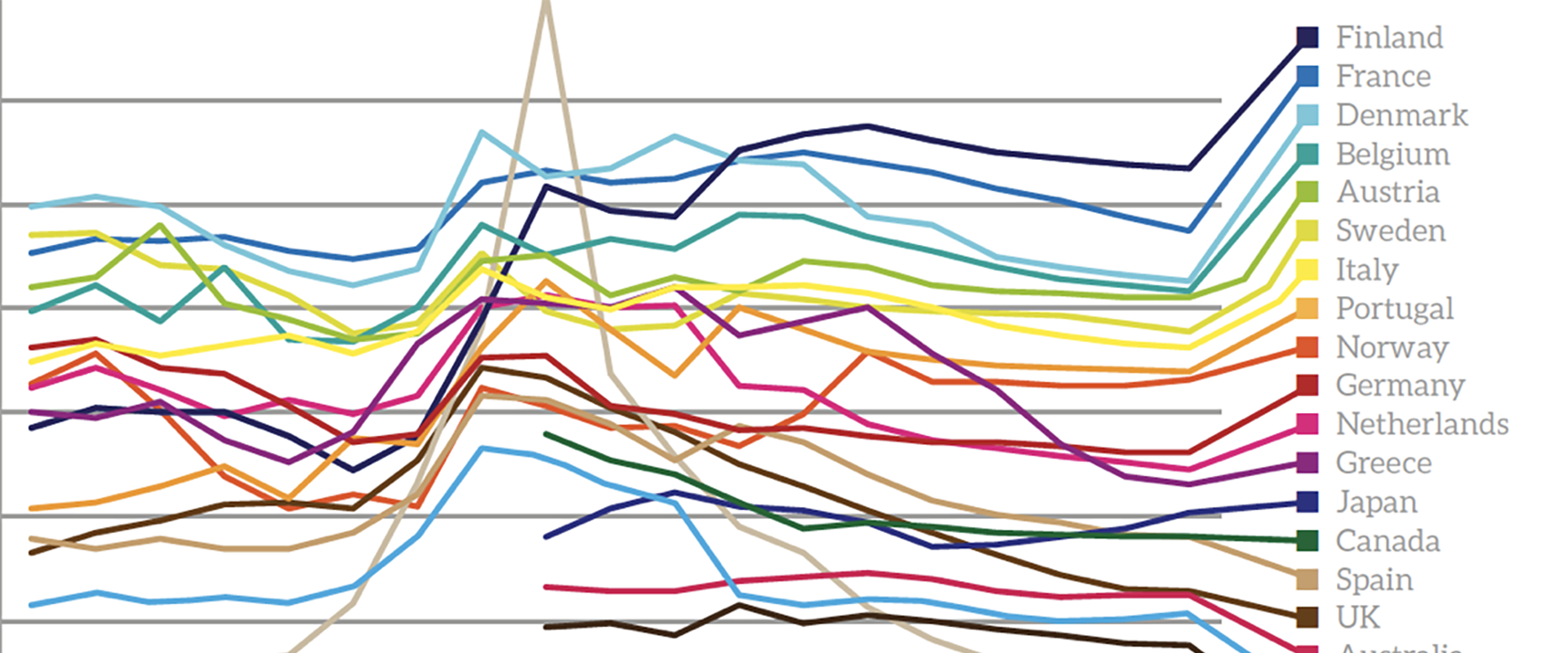
State Spending as a proportion of GDP for 20 countries, IMF estimates and projections